Some of New York’s largest and most prosperous hospitals are reporting rapidly growing amounts of revenue from pharmacy sales – most of it apparently flowing from a controversial drug discount program known as 340B.
The 34-year-old federal program allows designated providers to buy prescription drugs at steep discounts, ranging from 23 percent to 50 percent or more, while collecting full reimbursement from Medicare and other insurance plans.
Hospitals, clinics and other “covered entities” are free to keep the profits from these transactions without passing along the savings to their patients or accounting for much they collect – leaving policymakers largely in the dark about who is benefiting and how much.
However, some hospitals’ publicly available tax filings shed a little light.
As seen in the table below, at least four major downstate hospitals each reported more than $100 million in revenue from pharmacy sales in 2024 – amounts that have grown six-fold or more since 2019.
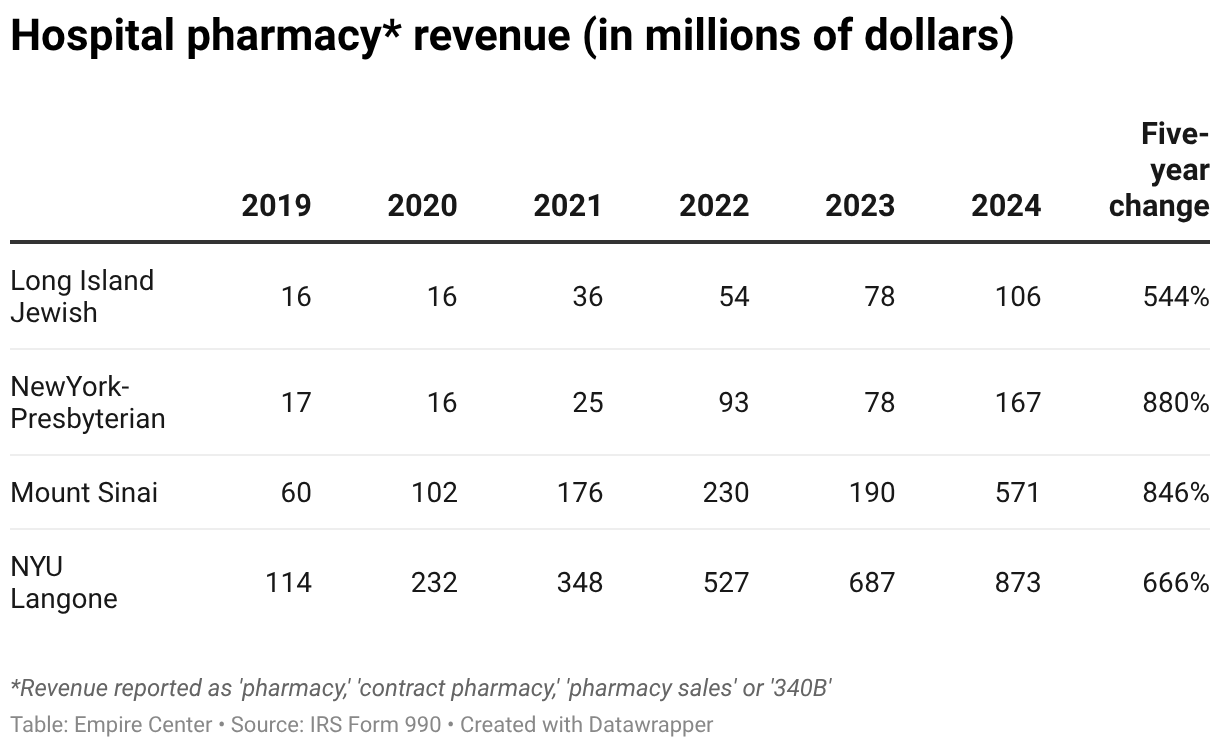
Not all of this money necessarily came from 340B. NYU Langone, for example, owns and operates a specialty pharmacy that would generate revenue regardless of federally mandated discounts.
However, Mount Sinai designated the relevant line item on its tax forms as “340B pharmacy.” NewYork Presbyterian called its line item “340B drug pricing” from 2017 to 2019, then switched to “contract pharmacy” after that – an apparent reference to the growing volume of 340B sales that flow through off-site retail chains instead of on-site hospital pharmacies.
These disclosures have implications for a policy debate currently unfolding in Albany: Legislation advancing in the state Senate – and included in the Senate’s budget proposal – would bar pharmaceutical manufacturers from trying to limit what they view as abuses of 340B.
If enacted, the bill would preserve a burgeoning source of cash for hospitals and clinics – but it would also drive up drug costs for consumers, employers and taxpayers.
When first enacted in 1992, 340B was targeted to a relatively small number of safety-net hospitals and clinics that directly dispensed costly drugs to indigent patients, such as people with HIV or AIDS.
Over the years, thanks to regulatory changes and court rulings, the number of “covered entities” in the program has ballooned from 500 to 13,000, including the majority of not-for-profit hospitals nationwide. Covered entities are applying the discounts – and reaping the profits – from a broad range of patients, including those with commercial insurance and high incomes. Rather than directly dispensing the medications, providers are increasingly contracting with third-party retailers to handle the sales.
The patients themselves don’t necessarily know that they are involved in the program. They don’t need to visit the covered entity regularly or even live in the same state, which is why hospitals in Manhattan and Rochester have 340B-related contracts with pharmacies as far away as Hawaii.
In 2024, 340B discounted sales totaled $81 billion nationwide, making it the second-largest federal drug program after Medicare Part D. The standard price for those drugs was about $148 billion, which resulted in an estimated $66 billion in net revenue for participating providers – 87 percent of which would have flowed to hospitals. (It’s unclear whether the total listed in the New York hospitals’ tax forms represent gross sales or net revenue.)
Defenders of 340B portray it as an important source of support for safety-net providers. In practice, however, it has become a broad, general subsidy that mostly flows to hospitals with little relation to need and minimal oversight.
The program also creates perverse incentives that have led to over-utilization of high-priced drugs and driven up the cost of cancer treatment.
Meanwhile, any drugs sold under 340B are not eligible for rebates that would otherwise flow back to insurers. That drives up drug costs for employer-sponsored health plans, including taxpayer-funded plans offered by state and local governments.
As 340B has mushroomed, pharmaceutical manufacturers have tried various ways to rein in what they view as abuses – by, for example, allowing covered entities to contract with only a limited number of outside pharmacies, or mandating that the pharmacies be located within a certain distance of the original provider.
In many states, providers have pushed back with “non-discrimination” bills that would require drug companies to grant all discounts authorized by federal law. New York’s version of that bill is sponsored by the Health Committee chairs in each house, Bronx Democrat Gustavo Rivera in the Senate and Westchester Democrat Amy Paulin in the Assembly.
Rivera’s bill has advanced through the Health and Finance Committees, setting up a possible vote of the full Senate. A version of it was also included in the Senate’s “one-house” budget plan, putting it on the table for three-way negotiations with Governor Hochul and the Assembly.
When the bill came up for debate in the Senate Finance Committee last week, several members expressed confusion about how 340B works – and frustration that they lacked clear information about how much money is flowing to which providers for what purpose.
Minnesota lawmakers have addressed some of those same concerns by ordering their state Health Department to gather data and publish a report. For 2024, Minnesota found that providers collectively bought $1.5 billion in discounted drugs, spent $165 million on operating costs, and collected $3 billion from insurers – resulting in net proceeds of $1.3 billion. Hospitals accounted for 98 percent of those sales.
The bulk of operating costs took the form of fees paid to contract pharmacies.
In the same spirit, a second piece of legislation in Albany – sponsored by Assembly Member Amanda Septimoe and Sen. Siela Bynoe – would require participating providers to disclose basic information about how they benefit from 340B sales.
Despite whatever good intentions its original authors had in mind, 340B has plainly morphed into a general-purpose cash cow that’s wasting money, driving up costs and distorting care delivery. As seen above, pharmacy sales that were not traditionally a major source of hospital income are now reaching into the nine figures for some New York institutions – amounting to 12 percent of total revenue for Manhattan’s Mount Sinai Medical Center.
Cleaning up the 340B mess is Washington’s job. What Albany lawmakers should be doing, if they want to make things better rather than worse, is demand a little transparency – and follow the money.







