I prescribed EpiPens yesterday, knowing they are overpriced. But I was shocked by how much.
This EpiPen I prescribed is for a mother who watched her 11-year-old son break out in hives from an insect bite on his arm. The hives then spread over his body. This time, fortunately, the hives did not spread to his throat or lungs. The next allergic reaction, however, can trigger a faster and fatal reaction in only minutes. It is hard to understate the emotions of a mother watching her child’s throat swelling.
EpiPens have doubled in price in just a few months, and now cost $300 or even higher.
There is not a shortage of epinephrine itself. But there are only a few suppliers of EpiPen and similar epinephrine injection devices to pharmacies. Access is controlled by a complex system of insurance middlemen exploiting the desperate need for this drug.
Anaphylactic allergic reactions cause suffocation and can easily be deadly. Patients are held hostage to their own health—they must pay for the epinephrine or risk fatal allergy attack. This is a public health emergency.
High costs are putting people’s lives at risk. Even insurance co-pays are often equal to or higher than paying cash. People are forgoing having life-saving epinephrine and taking their chances.
Nationwide, access to medications is restricted by the supply chain that is 85% controlled by four insurance corporations and their middlemen known as Pharmacy Benefit Managers (PBMs). These cartel-like conditions drive up drug costs, which are worse for critical drugs like epinephrine because people are desperate for them. Demand is high, the market is restricted, and inflation is the inevitable result.
The dose of epinephrine for anaphylaxis is 0.15 mg for children and 0.3 mg for adults. A 1 mg vial of epinephrine purchased for use in a clinic is only $10. Epinephrine is cheap; the devices are patented and controlled by our convoluted health care system.
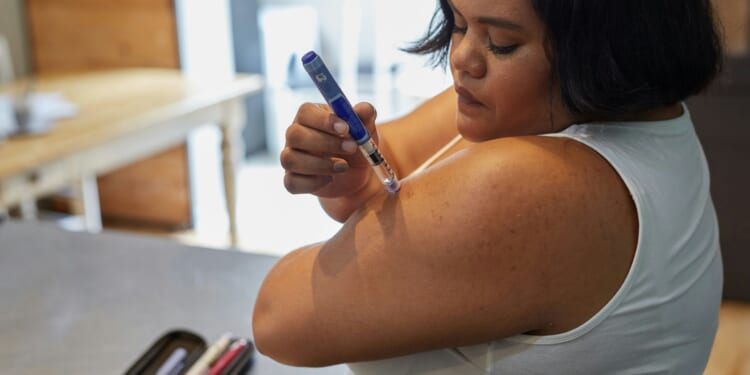
The solution is simple: We must change Texas law to allow physicians and independent pharmacies to directly supply patients with pre-filled syringes in a syringe carrying case. That $300 cost can turn into $10. For my cash-strapped patients, I will hand it out for free. In the U.S., patients already self-inject routinely with insulin and testosterone—and have for decades. But we can’t hand out epinephrine? A simple change of the law will save lives.
Other life-saving drugs are similarly cheap, but patients are paying highly inflated prices. Inhaled steroids for asthma and emphysema are cheap, but the inhaler devices are patented. Fluticasone is the generic drug in Flonase costs $10, but as the inhaler Flovent, it is $180. The wholesale direct cost to my clinic is $15 to $25. Severe asthma attacks are more common without steroid inhalers and can be deadly.
There are further outrages with biologic drugs for auto-immune conditions like rheumatoid arthritis that are thousands of dollars but should be only a few hundred.
Texas can no longer tolerate the exploitation of life-altering or life-threatening illnesses for the wealth of industry middlemen. The legislative changes are simple. There is no medical reason for blocking direct access to medications for patients from their doctors, or alternatives through independent pharmacies.
Reform is not hard, but resistance is staggering.